ECC Blog – Post-operative Free Fluid and Free Air by A-FAST in 22 Dogs Undergoing Ovariohysterectomy for Pyometra – April 2025
This is an interesting study out of Sweden that was published by Nilsson et al. in the journal Veterinary Radiology and Ultrasound in 2023. While checking out this study, I learned a wide range of things that were both related to what we teach, and the questionable thoroughness and attention to detail of the peer-review process. Before beginning this Blog or after this Blog be sure to check out “AFAST® and AUS in Septic Peritonitis” that further helps build your skills here.
- Our FASTVet 48-hour Rule for the Expectation of Free Blood in the Abdomen is Confirmed. Free Fluid Should Resolve or be Nearly Resolved within 48-hours Post-operatively.
- Lavage Fluid Lasts Much Longer – Lavage fluid may last up to 5-days or more.
- Free Air in the Abdomen Does Not Hinder Ultrasound Imaging.
- The Abdominal Fluid Scoring is Best Using AFAST® and in Lateral Recumbency here.
- Always perform abdominocentesis when free fluid is safely accessible. Abdominocentesis should be part of your skill set.
- The Peer-Review Process should always be critically evaluated by the reader.
- This is another of many examples of how are formats are not used the manner in which we teach them (thus, we service marked them [®] for educational purposes) – ie. the study is performed in dorsal recumbency and the abdominal fluid scoring system has not been validated in dorsal recumbency. The abdominal fluid scoring system is only valid in lateral recumbency.
- Get our 2nd edition textbook, Point-of-care Ultrasound techniques for the Small Animal Practitioner, 2021 here – it’s a great resource and read the POCUS Small Intestine Pancreas Chapter.
We will begin with the most recent and relevant, the Pyometra Study of 22 Post-op Dogs. No lavage fluid was used during then surgical event. However, these dogs were positioned in dorsal recumbency for “A-FAST Fluid Scoring” citing our study in the Methodology. This was only surprisingly discovered by my email to the author, Dr. Nilsson, who was kind enough to reply. The Reviewers never asked such questions.
My email commended their use of our AFAST®-applied Fluid Scoring System (let’s abbreviate AFAST® FSS) since it was used and better than reporting trivial, mild, moderate and severe, because AFAST® FSS gives much more information, i.e., the abdominal fluid score (AFS) that semi quantitates the fluid as small volume (<3) and large volume (>3) as well as designates locations that are positive and negative that may have some clinical relevance. See our Blog on our AFAST® FSS if you do not know its more recent (2015) modification with its “weak” and strong” positive AFS model here.

Screenshots of important text I have so that you may read and interpret in addition to my interpretation of findings. The study found that 45% of these dogs had small volume free fluid on Day 1 (versus 100% that received lavage fluid prior to surgical closure following small intestinal enterotomies in another study, Matthews et al. VRUS 2008). We have been teaching from the onset that lavage fluid is a confounder; and not only confounds, but it also lasts so much longer than blood [48-hours for blood, and 5+ days for lavage fluid).

So, always “dry” the abdomen prior to closure when lavage fluid is used. Use suction and then lift the mesocolon on the left and the mesoduodenum on the right to blot fluid with lap sponges (not gauze 4×4 that you can lose in the abdominal cavity leading to foreign body peritonitis) through the “gutters” as well as over the mid abdominal area as well.
“Free air” was also tracked. Recall that although “A-FAST” was used, these dogs were in dorsal recumbency, thus free air would rise to the midline. We teach right lateral and use of the Spleno-Renal (SR) view for “Free Air” because air rises to the least gravity-dependent region of the abdomen. Click here for the Detection of Pneumoperitoneum Webinar Short and Blog here.
Here is one of my teaching slides commenting on their table and findings:

Note that I have screenshot their summary Table and that time points were – Day 1, Day 4-6, and Day 10-15. Now you may see their findings. Note that it is unlikely that the “Free Fluid” was anything other than localized hemorrhage associated with minimal surgical trauma. It is resolved quickly, similar to our 48-hour FASTVet bleeding rule. At Day 4-6 100% were either negative (AFS 0), or were AFS 1. By email, the most common views were the CC and SR view according to Dr. Nilsson (unpublished, personal communication). Logic would dictate that the small volume assumed to be hemorrhage, was at the uterine stump (CC) and the left ovarian pedicle (SR); and likely these were even “weak” positives scored as “1/2” for those of you who have taken our Global FAST® Course here. The fluid was in too small a volume to be sampled and tested per the authors (thus my conclusion was very small “weak” positive pockets as we would conclude using our system, AFAST® FSS).
As for “Free Air” moving from Day 1 to Day 4-6 to Day 10-15 the “Free Air” was detected 95% to 82% to 14%, and it is reported to last up to 25 days in post-operative dogs, a study by Probst et al. in 1986.
For you and I, we need to know that “Free Air” is clinically relevant as follows: 1) it does not affect the AFAST® or a complete abdominal study (move the probe “under” then pocket of air, and 2) it is expected and should not be interpreted as a dehiscence (also you are combining other relevant clinical information on that patient when considering your assessment).
Hope you enjoyed this FASTVet Blog. Please send any comments to me, Dr. Greg Lisciandro, DVM, DABVP, DACVECC to FastSavesLives@gmail.com or LearnGlobalFAST@gmail.com. I do miss forms of messaging so please reach out again if I don’t reply within 48-hours.
********************************************************************************************************************************
Some other interesting earlier studies regarding “Free Fluid” and “Free Air” in the literature as an FYI.

Here is a graphed course of the presence of “Free Fluid”, “Free Air”, gastrointestinal motility, and brightness of surrounding mesenteric fat with my highlighting in colors because the original was too difficult to see without colors.
This illustrates how lavage fluid lasts “forever” compared to localized hemorrhage…

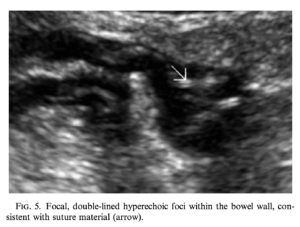
Interestingly, the sutures appear like heartworms with “=” signs. Furthermore, normal layering was not present for nearly all the dogs during the course of imaging. Another study followed even further out in time and normal layering still did not occur. My thought is the site has cicatrization so will always appear different than expected.
Hope you enjoyed this FASTVet Blog. Please send any comments to me, Dr. Greg Lisciandro, DVM, DABVP, DACVECC to FastSavesLives@gmail.com or LearnGlobalFAST@gmail.com. I do miss forms of messaging so please reach out again if I don’t reply within 48-hours.
gl/GL 4-3-2025